“People are going to die”
How the post-Roe world dawned on a Madison OB-GYN.
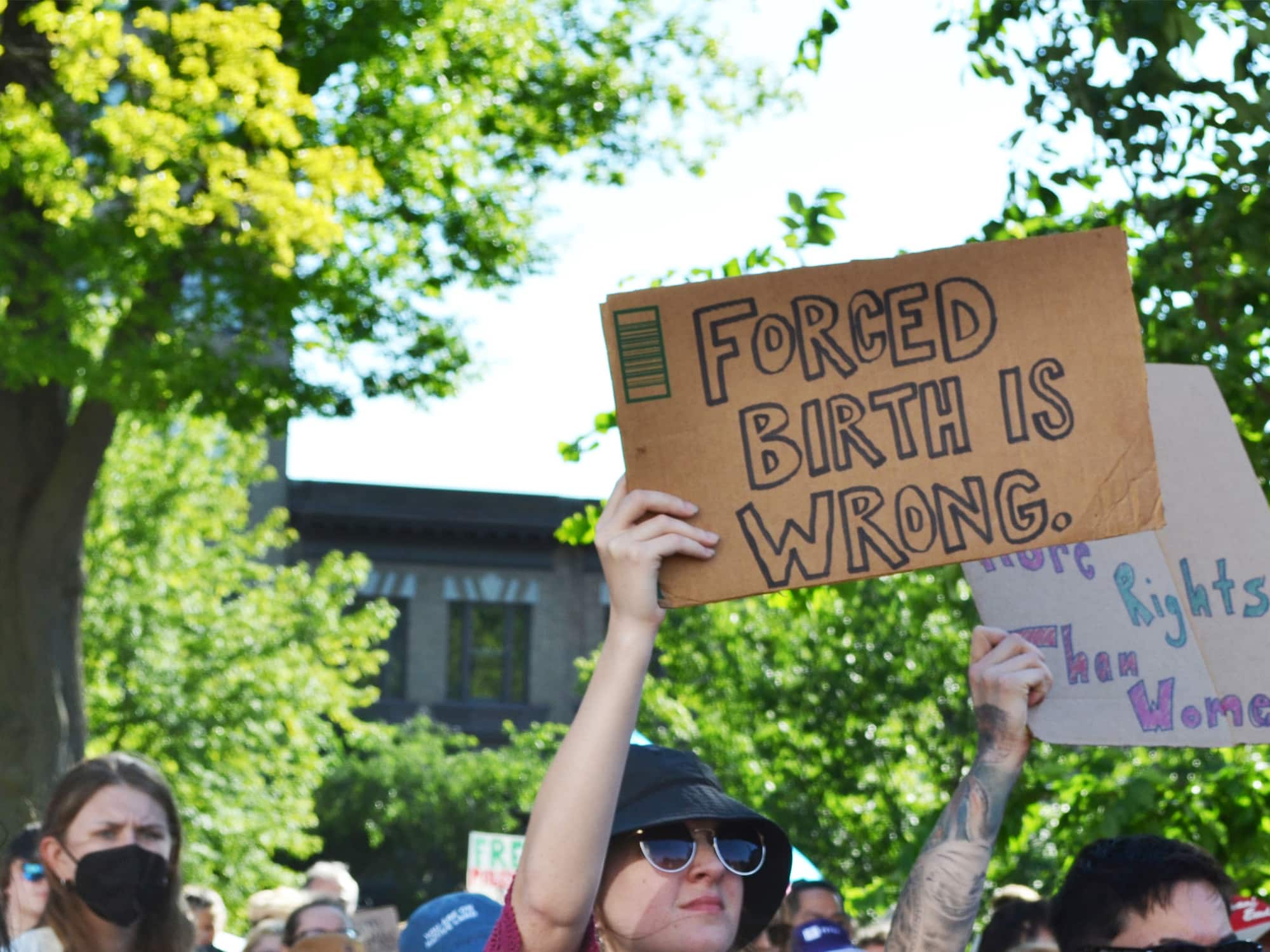
How the post-Roe world dawned on a Madison OB-GYN.
For Dr. Laura Jacques, a Madison-area OB-GYN, the impact of the Supreme Court’s decision to overturn Roe v. Wade was immediate.
Jacques had a patient scheduled for an abortion on Friday. The woman didn’t have the means to pay for the procedure, so Jacques’ team had scrambled to come up with the funds and schedule her before the final decision came down, which many suspected would be on the following Monday.
Instead the decision came down hours before her procedure. The patient’s fetus has no chance of survival, but she is now forced to carry it to term.
“That person was in my mind when it came down,” Jacques said. “It was immediate for one person. For many people, it was immediate.”
Planned Parenthood of Wisconsin announced earlier this month that it would not schedule abortions after June 25. On June 24 and 25, 70 abortions were scheduled. The organization said only four were completed before they stopped.
As of Friday afternoon, Planned Parenthood Advocates of Wisconsin stated its legal team was reviewing the decision and would post updates on what it means for the state.
Wisconsin’s 19th-century abortion law says that a physician who performs an abortion can be charged with a felony unless the life of a mother is in danger. But Jacques says legal teams across the state have been trying to answer doctors’ questions about how to determine when, exactly, an abortion would legally be considered “necessary… to save the life of the mother.”
“The whole thing is a gray area,” Jacques says. “We have been reviewing this law for months with every attorney you can imagine in multiple healthcare systems across the state… but what ‘threat to maternal life’ means is really unclear.”
What if the pregnant person learns they have cervical cancer? Can they abort to undergo radiation and chemo?
What if they have a heart condition with a 50% chance of surviving their pregnancy?
What if their water breaks four months into the pregnancy, which increases the risk of infection?
What about a patient who miscarries? Would they be able to prove in court that it was a miscarriage?
What about an ectopic pregnancy or a pregnancy outside the uterus?
“Any management of a pregnancy before 22 weeks, providers are going to be thinking about that within the context of this law,” Jacques says. “There is not a single physician who takes care of pregnant people in the state who is not thinking hard all day today [Editor’s note: the interview took place Friday afternoon], all day going forward about whether the care they’re giving is going to be a threat to the patient. Is it enough of a threat to the patient? Is it too much of a threat to themselves?”
Jacques recalls one case she had where the pregnancy had exacerbated an unknown heart condition that made the patient so ill she was unable to drive, work, or care for her children.
“We had one day in the month where she could find somebody who could drive her to the hospital to take care of her and to end this pregnancy that would’ve killed her,” Jacques says. “[Now] what’s going to happen to that patient? There’s no way that patient’s going to be able to make it to another state.”
“People are going to die,” Jacques says. “This is not hyperbole. It sounds like hyperbole, but I can think of the people that would’ve died if we hadn’t been able to provide care. And those people are now going to—they’re not going to make it.”
Jacques saw a preview of a post-Roe world during the pandemic. She researches decision-making around abortions and continued that research as some states used COVID-19 safety protocols to ban abortions, deeming them “elective” procedures.
Her team reviewed Reddit posts where people tried to figure out how to safely access abortion; which websites would provide medication, would they arrive in time, would the medicine that arrived be the same they ordered, etc.
There was one woman whose medical abortion (via pill) didn’t work, and she couldn’t figure out who was going to look after her children so she could make the trip across state lines. There was another who was in an abusive relationship and felt “trapped and desperate” because she couldn’t figure out how to terminate her pregnancy.
Jacques also researches decision-making around fetal anomalies—situations where families wanted the pregnancy, but something had gone horribly wrong.
“They all referred to it as their baby [and] spoke about the child by name. These aren’t decisions that people make lightly,” she says. “And now to have to tell people that we can’t help them, it just adds more pain to the suffering that they’re already going through.”
Who has power in Madison,
and what are they doing with it?
Help us create fiercely independent politics coverage that tracks power and policy.




